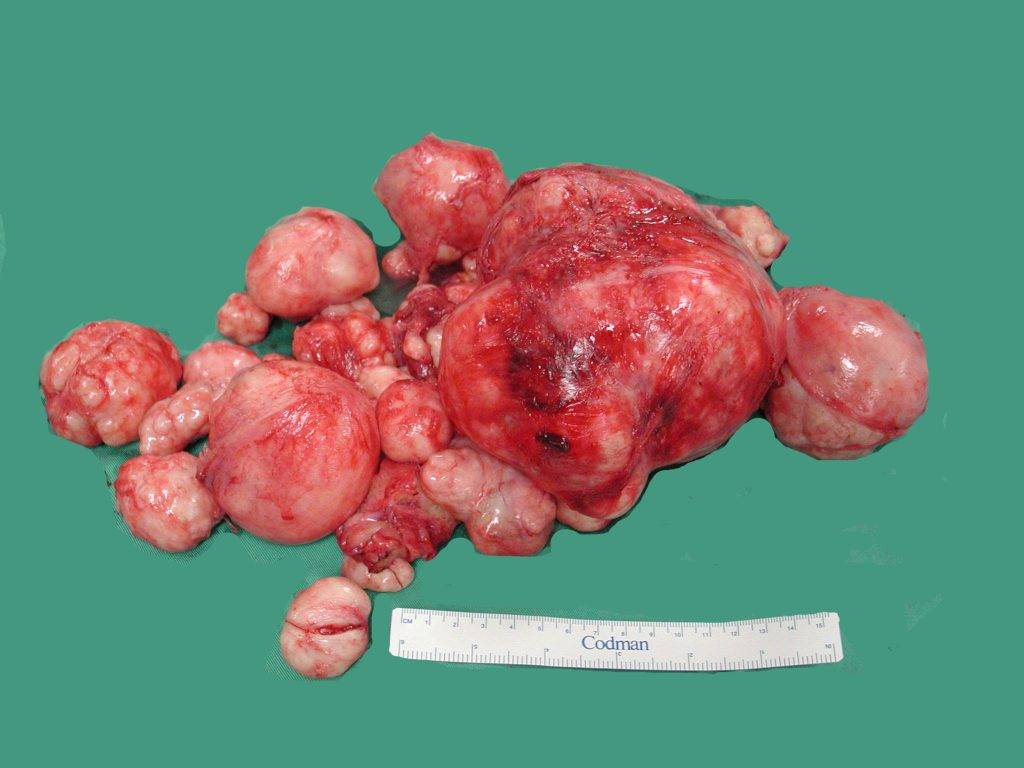
Fibroid… Threat to female reproductive health
“It is not my time of the month, what is wrong with me,” was the question Setriakor (not her real name) asked herself as she looks at her blood stained dress.
As the days went, the flow was heavier with thick dark clots, for which her usual pad could not sustain. She later resorted to the use of diapers. That also failed to absorb the amount of blood and clots ‘gushing out.’
She dares not laugh, cough or do any strenuous activity, lest her dress will be soiled, wherever she finds herself.
Setriakor, a 36-year old Scripter, looked pale and found it difficult to work for a number of weeks.
She decided to visit a local Chemist to explain her ordeal. In the end, a blood tonic was prescribed for her with the hope to replenish the lost blood.
He also advised her to visit the hospital to see a doctor.
Her visit to the health facility the following week ended up with the gynaecologist who performed a scan on her. The results of the scan revealed she had multiple fibroids.
Suddenly, all the stories she had heard about fibroid began racing through her mind. It took a lot of counselling from the gynaecologist to calm her down.
This is the challenge most young and adult women go through with some either losing their uterus or life in the process due to delay in seeking medical attention.
Fibroid, is non-cancerous growth that develops in or around the womb or uterus. The growth or growths are made up of muscle and fibrous tissue. They vary in size.
Many women are unaware they have fibroids because they do not have any symptoms.
Women who do have symptoms of fibroid are likely to experience heavy or painful periods, abdominal pains, lower back pain, frequent urge to urinate, constipation and pain or discomfort during sex.
Women who are diagnosed of fibroid often undergo hysterectomy in order to have it removed.
Most women of African-Carribean origin tend to develop fibroids more frequently and are common with around one in three women.
Types
The Chief Executive Officer of Ladybits Health and Wellness Clinic, Dr Victoria Partey-Newman in an interview with The Spectator said there were four types of fibroids which can occur in women.
The types, she said, were intramural, subserosal, submucosal and pendunculated fibroids.
She explained that intramural fibroids occur in the wall of the uterus. This type of fibroid grows quite large.
Subserosal fibroids grow outside the uterus and may press on other organs of the pelvic area.
Submucosal fibroids grow beneath the lining of the uterus and grow into the uterine cavity which is the central part of the uterus.
“Submucosal fibroids can make it harder for one’s uterus to support conception and maintain pregnancy,” Dr Partey-Newman stated.
According to her, submucosal fibroids are most likely to cause painful cramping as well as bleeding between periods.
Pedunculated fibroids are mushroom-like and grows at the end of small stalks within or outside of the uterus. When the stalk of a pedunculated fibroid become twisted, it can cause intense pain.
The uterine fibroids, however, are the most common tumour in women and very prevalent in infertility issues.
Infertility
Dr Partey-Newman said fibroids could be the sole cause of infertility in two to three per cent of women but the exact cause is unknown. It has often been linked to the hormone oestrogen.
Oestrogen is the female reproductive hormone produced by the ovaries.
Dr Partey-Newman said fibroids most often develop between the start of puberty and menopause, adding that the risk increases with age.
According to her, having a family member with fibroids could increase one’s risk of having it but said “you should not discount the symptoms simply because you do not have a family member with fibroids.”
She said fibroids cannot be prevented but can reduce risk by maintaining a healthy body weight and have a regular pelvic examinations.
Treatment
Dr Partey-Newman said surgery was not the only option for the treatment of fibroids.
They can be treated with medication.
Currently, Gonadotrophin-releasing hormone (GnRH) agonists and selective progesterone receptor modulators (SPRMs) are the most effective medical therapies with the most evidence to support the reduction of fibroid volume in menstrual bleeding.
Another way to treat fibroid was uterine fibroid embolisation which is done by cutting off blood supply to the fibroids. That causes them to shrink.
Dr Partey-Newman, however, said “if symptoms do not improve with medication or nonsurgical treatment, or if the gynaecologist suspects fibroids may be causing infertility, surgery may be the next treatment option.
“The goal of surgery may be to relieve pain, reduce menstrual blood flow, or improve fertility.”
Advice
She said since fibroids could reoccur after surgery, it was important for women to quickly get married and start making babies, especially those who have had their fibroids removed.
“In our society, where men are the ones that propose mostly, it somehow makes it difficult for women to marry early and start giving birth.
That contributes in making the fibroids recur again.
She advised women to visit the hospital when they notice changes in their reproductive cycle and urged them to adhere to doctor’s advice when diagnosed of the disease.
She cautioned that women diagnosed of fibroids must avoid herbal concoctions which could affect their kidneys in the long term.
By Jemima Esinam Kuatsinu